Due to predictable pharmacokinetics and pharmacodynamics, patients receiving LMWH therapy do not require routine coagulation monitoring. Despite this, there is some concern that a fixed or weight-based dosing of LMWH may put certain patient populations at risk for suboptimal effectiveness and safety. Data are lacking regarding the clinical utility of anti-Xa-guided dosing in patients receiving LMWH for VTE prophylaxis. The goal of this study is to evaluate relevant thromboembolic or bleeding outcomes for patients within 30 days of initial treatment with LMWH.
This retrospective cohort study evaluated patients from the University of Utah health system receiving enoxaparin for VTE prophylaxis between September 1, 2018, and September 30, 2019. Patients were evaluated for the occurrence of bleeding or thromboembolic adverse events. The primary outcome for this study is the composite of any VTE, International Society of Thrombosis and Haemostasis major bleeding, and mortality in the 30 days following the initial enoxaparin dose in patients either receiving or not receiving anti-Xa monitoring. Secondary outcomes were the individual components of the composite outcome.
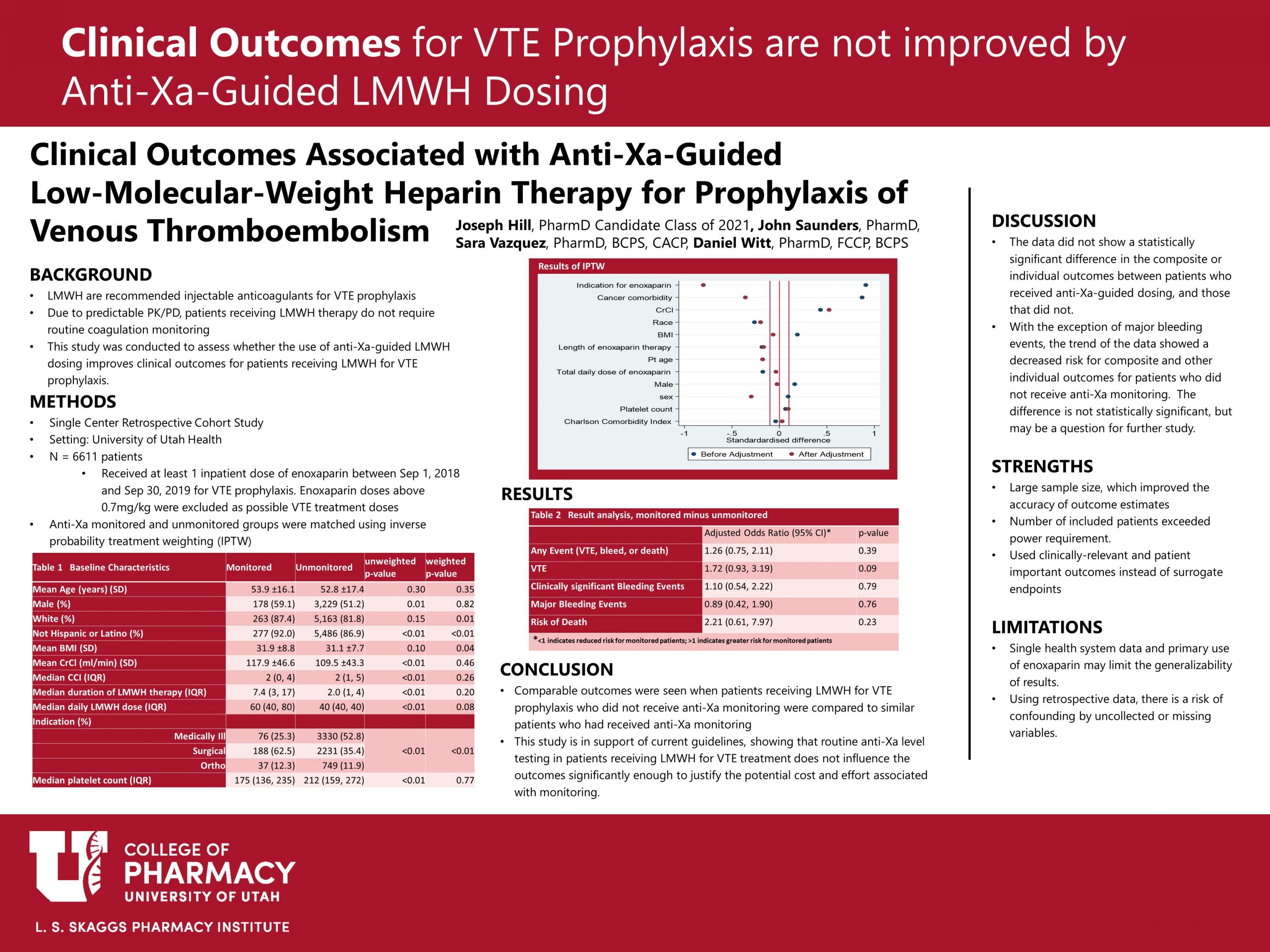
During the 13-month analysis period, a total of 6611 patients were analyzed for VTE or bleeding events. IPTW allowed matching of patients between those who received anti-Xa monitoring, and those that did not to control for confounding variables.
Patients receiving LMWH for VTE prophylaxis with anti-Xa monitoring were associated with higher odds of experiencing a composite outcome of VTE, bleeding or death from any cause. For individual components of the composite outcome, the odds of any adverse outcome did not increase in the unmonitored group. This evidence supports current evidence-based guidelines that recommend against routine anti-Xa monitoring



Responses
Joe – very interesting work. This is just comment, not a question. I see that the weighted P-value of the two groups are not significant mostly but there remains statistically significant differences for some variables e.g. white, mean BMI. I wonder if this might be due to by chance. I wonder if you can present the SMD to compare the weighted and unweighted data as it is more common these days to present it since it gives us magnitude of the differences rather than relying on statistical significance which might not be clinically meaningful. What do you think about this?
Great question! My first thought is that this would be due to chance, but I would honestly need to look into the data a bit more to formally make a conclusion. I think at this point our plan is to include all of the supplemental information in an appendix with the article.
Nice work, Joe. Based on the results of your study, what would you say to a physician who wanted to order anti-Xa monitoring on a patient receiving VTE prophylaxis?
At first thought, I would try to dig deeper and see what it is the physician is really questioning. Is it the efficacy of the treatment? Do they just want reassurance? I would also ask them what they planned on doing with the anti-Xa level. Hopefully, I would be able to reassure the physician and ensure that the patient is getting the best treatment.
Interesting. Thanks.
Thanks for coming and taking a look!
Good work, Joe! Based on your findings, what do you think a follow-up study should be? What warrants further/more definitive analysis?
It would be interesting to look further into whether anti-Xa monitoring decreases the bleeding risk in patients receiving VTE prophylaxis. The data was not significant, but it may be worthwhile to look more into that observed trend.
Joe, nicely done. Your work is quite interesting, and I found your poster well organized and easy to follow. Thank you for presenting the work so clearly!
Thank you so much! There was a lot of help and input from the whole team, but I think it turned out well too!
Comments are closed.