Abstract
Introduction
The opioid epidemic is a national health crisis that is increasing opioid overdose deaths every year. Opioids are commonly used post surgeries for pain management, but how has opioid utilization changed over the past few years in response to the rising overdoses?
Methods
Prescription rates for opioids written between 30-90 days post discharge from TKA operations were collected over a 5-year period. Data were collected via procedural codes from a data warehouse, and a random sampling of 100 patients was selected for data analysis. Utilization rates were analyzed using descriptive statistics and opioid demographic information was presented.
Results
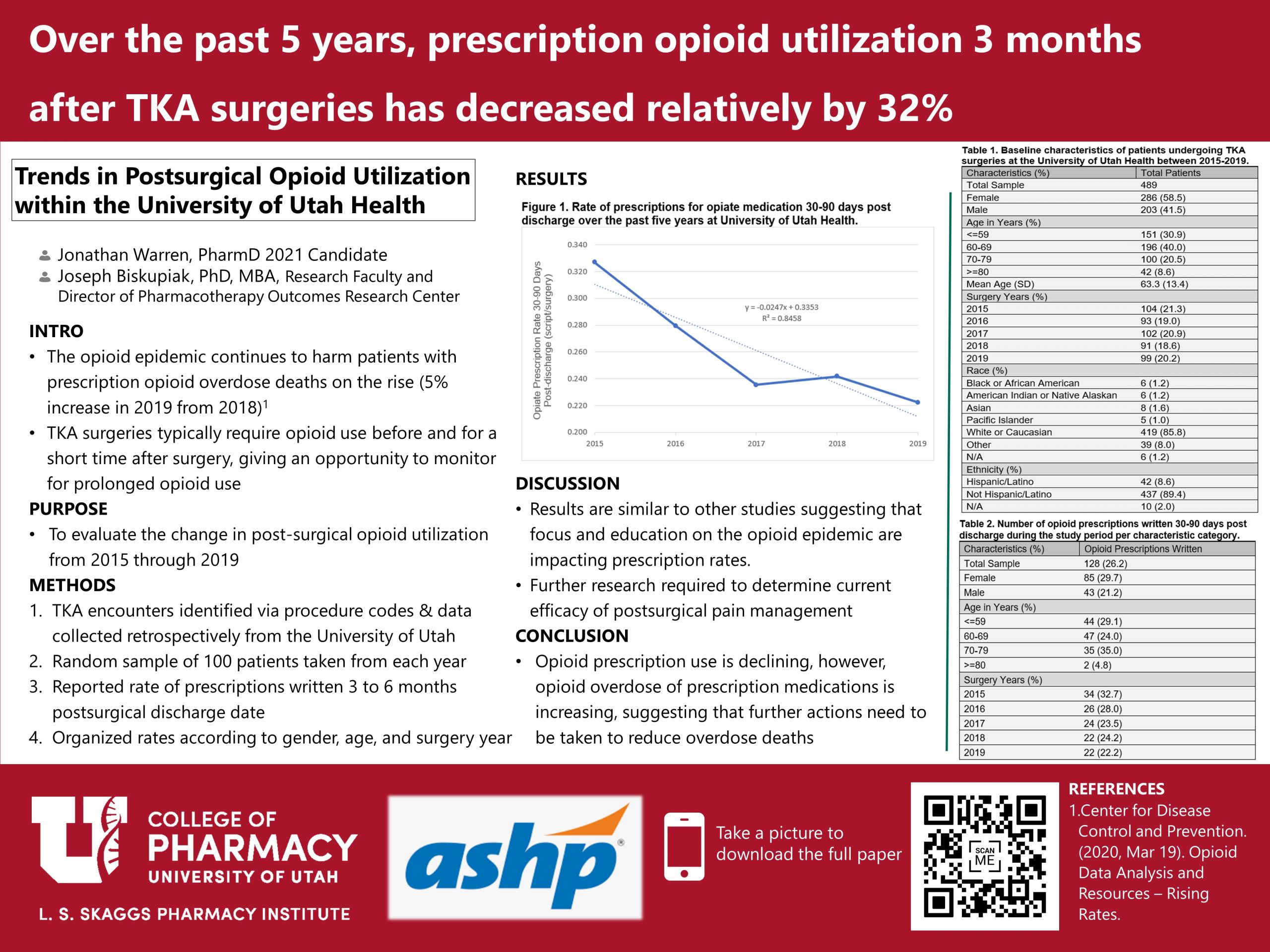
The rate of opioid utilization had an absolute decrease of 10.5% from 2015 to 2019, which is a 32.11% relative reduction, and had an average decline of 2.47% each year. The opioid utilization rate was slightly higher in females than males (29.7% vs. 21.2%). The ages with the highest rate were age 70-79 years (35.0%) and age <60 years (29.1%).
Conclusion
This study demonstrated evidence that opioid utilization 30-90 days post-discharge from orthopedic surgery has been declining over the past 5 years.



Responses
Excellent poster! I’m glad to see opioid prescribing decreasing in this setting.
Nice work Jon! With the decreasing trend in opiate use, were then increasing trends in the use of non-opioid analgesics like NSAIDs? Any thoughts about what might happen to post-surgical bleeding rates if surgeons are replacing opiates with NSAIDs which have anti platelet effects?
Thank you for the questions! Unfortunately, non-opioid pain management use was not evaluated in our study. However, the rate of specific non-opioid pain medications, like NSAIDs, would be an interesting topic for further study. While it is assumed that these other options are increasing in utilization, some studies of certain surgery types have shown decreases in opioid use without the need to increase other pain medications.
Use of NSAIDs in postsurgical pain management can have complications due to increased bleeding risk. If physicians were directly switching from opioids to NSAIDS, this would be very concerning and would likely increase post-surgical bleeding rates. However, there have been some recent studies suggesting that increased use of NSAIDs (Cox non-selective and especially Cox-2 selective) in specific types of surgeries has not resulted in increased adverse bleeding events. Still, careful consideration of the patient’s individual risk factors and the surgery bleeding risk is needed before NSAIDS should be used.
Interesting. Scary the older one gets the more increase in opioid use.
Nice work, Jon! It is heartening to hear that prescriptions for post-surgical opioids are going down, particularly for those being written longer-term after the procedure. Do you have a sense as to what is is about these ~25% of patients that receive a prescription for an opioid >30 days post-op? Is there some characteristic that might allow one to better address the continuing use in this population?
Great questions! Although we were able to exclude any patient with a cancer diagnosis, patients on chronic opioid therapy for other indications such as lower back pain were still included in the sampling. It is expected that a significant portion of that 25% still on opioids would be the base rate of patients on chronic opioid therapy. Future study into this specific patient population (those continuing opioids >30 days post-discharge) could help determine the true rate and causes of prolonged post-surgical opioid utilization (ex. complications from the surgery, poor wound-healing comorbidities, potential abuse, etc).
Hi Jon! Great research topic and great conclusion to that research!! I am glad that these prescription rates are declining. I wonder which drugs, however, are now being prescribed more often (gabapentin?). Nice work on the poster, too! Easy to grasp ideas and findings! Thank you for sharing your research!
Comments are closed.